3DHEALS 2017 Takes the Temperature of 3D Printing in Healthcare

Jennifer Chen M.D., founder and CEO of 3DHEALS, which focuses on 3D printing in healthcare (image courtesy of Jennifer Chen).
Latest News
April 11, 2017
 Jenny Chen M.D., founder and CEO of 3DHEALS, which focuses on 3D printing in healthcare (image courtesy of Jennifer Chen).
Jenny Chen M.D., founder and CEO of 3DHEALS, which focuses on 3D printing in healthcare (image courtesy of Jennifer Chen).Though originally a rapid prototyping technology for engineers and designers, 3D printing has also attracted the attention of doctors, dentists, and surgeons. The technology offers new ways to produce prosthetics, implants, and artificial limbs. Therefore, a partnership between 3D printing and healthcare is not an unlikely marriage.
3DHEALS 2017, a conference taking place in San Francisco next week (April 20, Mission Bay Conference Center), will explore the link between the two. This is the fifth conference curated by the organizers.
Cautiously Optimistic about 3D Printing in Healthcare
Wohlers Associates Inc., an analyst firm that specializes in 3D printing or additive manufacturing (AM), recently published its 2017 market report. It reveals the medical and dental segment contributed $667 million of the market’s total revenues of $6.063 billion in 2016. At roughly 11% of the total, the contribution is not negligible.But if AM vendors want to court the healthcare industry, they may have to do a much better job in outreach, education, training, and user interface redesign.
Jenny Chen, a trained neuroradiologist and the founder/CEO of 3DHEALS, says, “Most healthcare providers’ knowledge on AM or 3D printing remains limited on what is available in the media, i.e. some high-profile user cases ... Currently, systematic 3D printing education in healthcare is only available to selected dental schools, residencies, and a few CME (continued medical education) courses, like the Mayo Clinic and RSNA (Radiological Society of North America). Even with these educational programs, the curriculum is still in its infancy as the teaching institutes are continuing to learn about the technology themselves.”
The adoption of AM in healthcare also depends on regulatory and institutional acceptance. The U.S. Food & Drug Administration (FDA) has begun certifying certain 3D printing materials and processes for medical use. (For more on this subject, read “Materials: 3D Printing’s Medical Miracles,” October 2015).
“Healthcare is a highly-regulated field, for good reasons,” says Chen. “There are quite a few concerns that the additive manufacture industry and healthcare professionals need to address before the technology can be fully implemented. These include: material safety/toxicity (esp. in biological systems), manufacturing standards (including safety and quality control), liability, and efficacy.
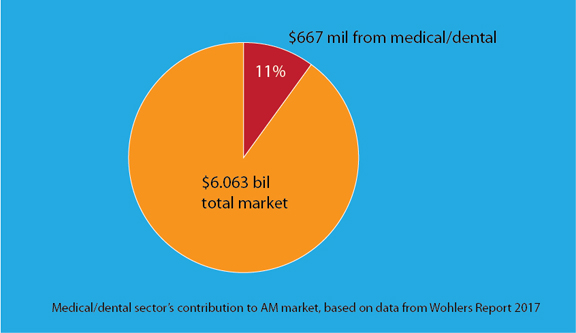 According to Wohlers Associate’s 2017 report on the 3D printing market, the medical/dental sector contributed roughly 11% to the overall market revenue (chart created by DE based on data from Wohlers Assoc.).
According to Wohlers Associate’s 2017 report on the 3D printing market, the medical/dental sector contributed roughly 11% to the overall market revenue (chart created by DE based on data from Wohlers Assoc.).The Doctor’s Prescription
Chen has a wish list—a set of pills that would make 3D printing easier to swallow for the medical professionals. Here is her list, in her own words:- Price. Of course, the cheaper the better. Decreased overhead (both software, hardware, and materials) will create more room for creative use cases, which will result in an increase in demand. However, it is notable that in healthcare, absolute price is often not the most important factor. For example, if a 3D-printed hip implant costs $1,000 more but lasts 5 years longer than the traditionally made implant, I think the cost is justified.
- Software. 3D printing software has made significant improvements over the past 10 years, and in user interface in the last three years. This is a result of increased computing power as well as increased investment from software companies in the healthcare vertical. I anticipate more one-push solutions for both existing and new software in healthcare.
- Material. We don’t have enough selections in bio-compatible materials. This is partly due to limited use cases and toxicology profiles on many existing AM materials. Both require time and money. Dr. Steven Pollack (senior research scientist at Carbon) recently wrote a very nice article on the subject.
- Applications. There are increasing numbers of new 3D printing applications in healthcare, which is evident based on a simple literature search on PubMed. However, many of these applications are limited to small populations or one-off cases. Both healthcare and 3D printing industries need to invest more to find the best intersecting applications.
- Education. Lack of application is partly due to lack of education. This applies to both the engineering/industry side and the healthcare provider side.
Subscribe to our FREE magazine, FREE email newsletters or both!
Latest News
About the Author
Kenneth Wong is Digital Engineering’s resident blogger and senior editor. Email him at [email protected] or share your thoughts on this article at digitaleng.news/facebook.
Follow DE